

In vitro fertilisation
(IVF, «test-tube babies»)
Since 1978, when Louise Brown was born in England, this method to bring together egg and sperm in the test tube has already been in use. Originally, IVF was developped to treat women with blocked Fallopian tubes; nowadays, IVF is also an effective method to treat moderate male fertility problems, endometriosis and unexplained infertility. World-wide over four million healthy babies have been born. Contrarily to sperm/egg donation and adoption, mother and father are genuine biological parents of the child. A pregnancy after IVF has a normal course, provided it is a single pregnancy.
IVF and the micro-injection ICSI (see dedicated page) are methods of so-called assisted reproduction. In those methods, the quality of the laboratory plays a pivotal role. Our practice has a long-standing collaboration with the excellent biological team of Professor Brian Dale, whom I have the privilege to know since 1999. All IVF specialists and laboratories are regulated by the Swiss Law on reproductive medicine, and the Confederation imposes a mandatory quality control. Egg retrieval and embryo transfer necessitate an outpatient clinic stay of one to two hours each. Depending on the medical situation, success rates vary from 20 to 40 percent per attempt.
Contrarily to our neighbouring countries, methods of assisted reproduction are unfortunately not covered by Swiss health insurance, which will remain so in the foreseeable future. Our very competitive basic price is 5900 Swiss francs, including anaesthesia for egg collection, and including intracytoplamic sperm injection as well (excluding medication to stimulate the ovaries, whose consumption greatly varies from one individual to another). A thawing cycle costs approx. 2000 francs.
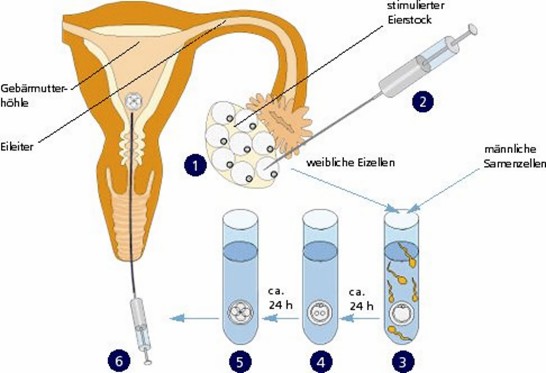
Top: Principle of IVF method
(from Organon brochure)
1. Ovary, stimulated by hormone injection to produce several follicles at a time
2. Transvaginal egg retrieval in ultra-short anaesthesia
3. Egg and sperm united in the test tube
4. The next day: fertilised egg (zygote)
5. The second day: embryo in four-cell stage
6. Transfer of the embryo in the uterus (no anaesthesia needed)

Excess fertilised eggs («zygotes», number 4 in the topmost picture) can be frozen - upon request of the couple - in liquid nitrogen at -196 degrees Celsius (cryopreservation). The picture on the top shows an opened storage container. Thus the patient gets a second chance to get pregnant, in case the first («fresh») attempt was unsuccessful; during this second chance, she needs not to undergo ovarian stimulation and egg retrieval, and the cost is substantially lower.
The two weeks of waiting time after embryo transfer are considered the most burdensome phase of treatment by many couples. Then we perform a blood test for pregnancy hormone, whose result is available the same day.
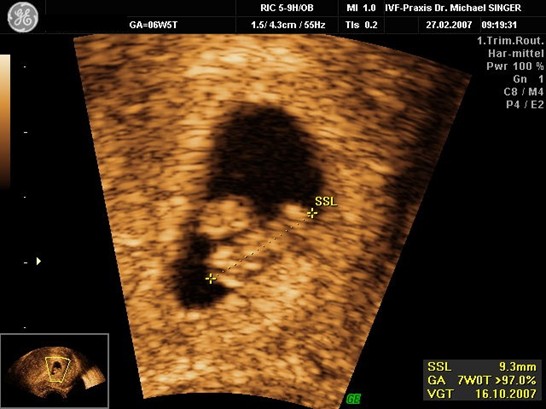
This is the outcome the patient was dreaming of during her long treatment: five weeks after embryo transfer, we see on ultrasound an single embryo of nine millimeters with clear heartbeat inside the patient's womb. The patient is pregnant!